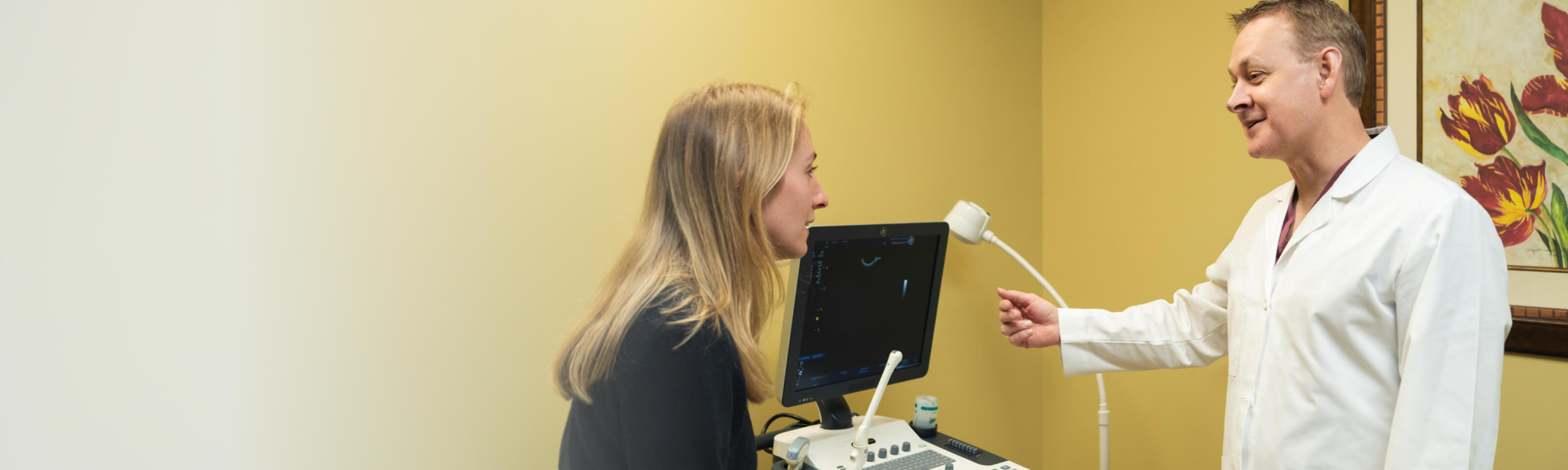
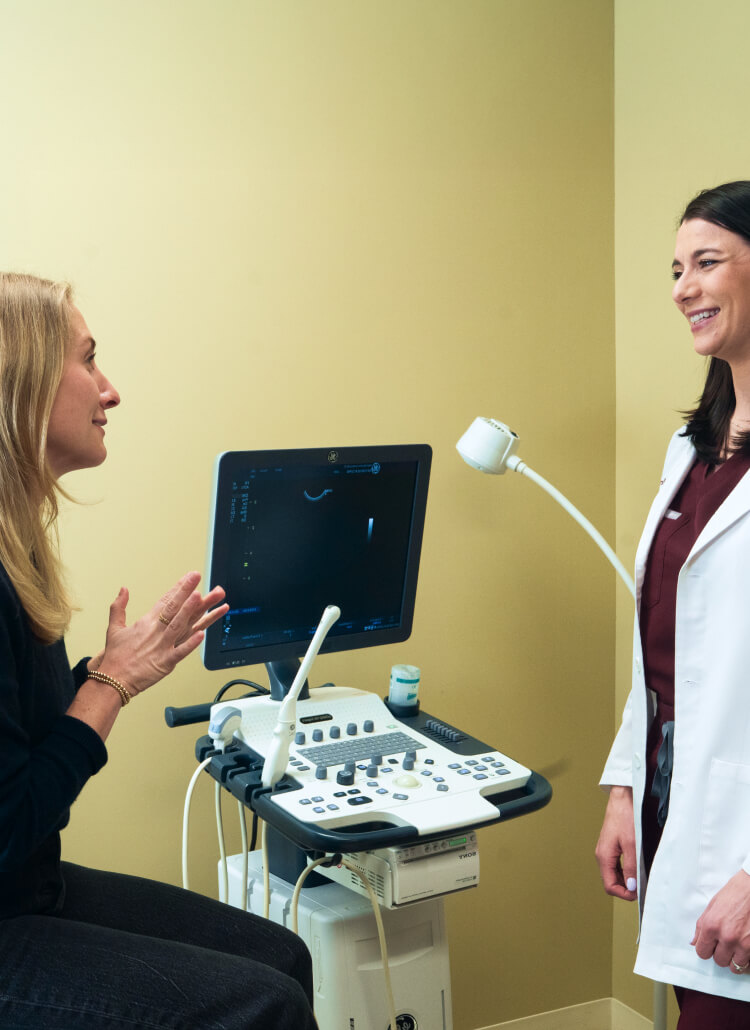
When you’re trying to grow your family, answers matter. Because infertility can stem from one or both partners, we take a comprehensive approach to fertility evaluation. This means testing both partners early on — helping us identify potential issues and recommend the best path forward with care, clarity, and compassion. Below is an overview of the fertility evaluations we perform for female patients.
Follicular-Phase Blood Tests & Egg Quality Assessment
One of the key ways we assess a woman’s fertility is by evaluating her ovarian reserve – the number of immature eggs remaining in her ovaries. Every woman is born with all the eggs she’ll ever have, and that number naturally declines over time. We accomplish this by measuring the hormones AMH (Anti-Mullerian Hormone). FSH (Follicle Stimulating Hormone) and estradiol (E2) on the second, third, or fourth day of the menstrual cycle.
The FSH and E2 results help us determine whether more advanced treatments should be recommended and how likely we are to achieve a successful pregnancy using the patient’s own eggs.
Endometrial Lining Assessment & Biopsy
A healthy endometrial lining – the inner layer of the uterus – is crucial for embryo implantation. During the first half of the cycle, estradiol helps thicken the lining. After ovulation, progesterone takes over, enriching the lining and making it receptive to a fertilized egg.
In some cases, the uterine lining requires evaluation by an endometrial biopsy, usually performed just before the onset of menstruation. This helps us identify any issues that might interfere with implantation. Research continues to explore how conditions like endometriosis or immune system factors may impact this process, including possible deficiencies in the proteins that help embryos anchor to the uterine wall.
Hysterosalpingogram (HSG)
The hysterosalpingogram (HSG) test is a specialized X-ray used to examine the uterus and fallopian tubes. It helps confirm that the fallopian tubes are open and that the uterine cavity is free of blockages or abnormalities. This test is typically performed between days 6 and 13 of the cycle, after menstruation has ended but before ovulation. Some cramping or discomfort may occur during the procedure.
FemVue
FemVue is a non-invasive diagnostic procedure used to assess whether the fallopian tubes are open, which is an important part of fertility evaluation. Unlike traditional hysterosalpingography (HSG), FemVue combines saline and air bubbles with transvaginal ultrasound to visualize the movement of fluid through the fallopian tubes. The procedure is typically performed in an office setting and takes only a few minutes. During the test, a small amount of sterile saline and air is introduced into the uterine cavity through a thin catheter. The movement of the air-saline contrast is then monitored in real time using ultrasound to determine if the fluid flows freely through the fallopian tubes.
Saline Sonohystograms (SIS)
Saline Sonohysterogram (SIS) is a specialized ultrasound that uses sterile saline to evaluate the inside of the uterus. It helps detect polyps, fibroids, scar tissue, or uterine abnormalities that may affect fertility. The procedure is quick, well-tolerated, and avoids the use of X-rays or contrast dye. It is performed in-office early in the menstrual cycle with minimal downtime.